1. WELCOME AND APOLOGIES
PRESENT:
Patients: Gill Walt (Chair), Mimi Colahan (Vice Chair), Judy Hildebrand, Kirsten de Keyser, Nori Graham, Isky Gordon, Veronica Brinton, Adrian Davis.
Staff: Sarah Worboys, Jamil Ahmed
APOLOGIES:
Ian Critchley, Donatella Soldi, Kathy Graham-Harrison
2. COMMUNICATION BETWEEN PATIENTS, PHARMACIES AND PRACTICE
Prescriptions
Patients on the PPG email list were asked for their experiences with prescriptions, and these were then collated. The main problems identified were:
- Re-ordering repeat prescriptions. Some pharmacies automatically send the next batch of medication, but others make you re-order yourself on-line.
- Getting medicines ‘synced’ – ordered together rather than in separate batches
- Wrong prescriptions sent; repeat prescriptions not updated; problems when changing a medication within a repeat prescription
Most of the issues raised were known to the Practice, and attempts are being made to address them with the various individual pharmacies – a project in progress. Through her presentation of the way the prescription system works, Dr Worboys gave a number of examples of how complex the prescribing of medicines can be. She emphasized that GPs are held individually responsible for their prescribing, and that the Practice is trying to move from paper prescriptions to electronic prescribing which is safer. She presented a flowchart of how the system works:
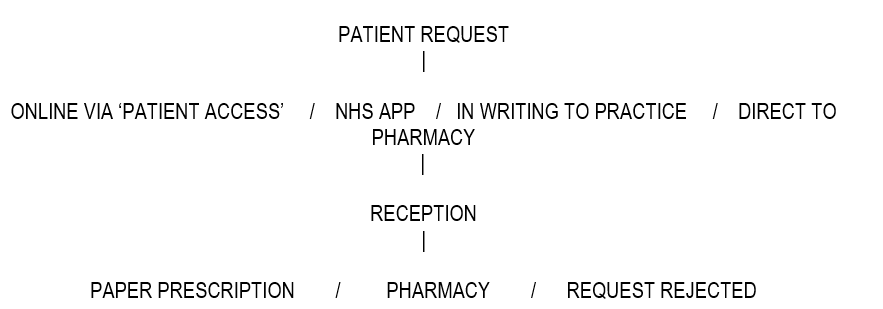
That is, patients can request their prescriptions in 4 ways:
- online via Patient Access (only for repeat prescriptions)
- via the NHS App (only for repeat prescriptions)
- in writing to the Practice
- directly from the pharmacy
No requests for prescriptions can be made on the telephone, because the opportunities for errors are too great. All requests go to reception staff who pass them on to the doctors, for checking. Pharmacy requests also go to reception staff because sending them directly to the doctor can delay the process (for example, if the doctor is away). Patients usually nominate a specific pharmacy of their choice. It is possible for the Practice to send prescriptions to other pharmacies in England (eg if patients are away from home).
Dr Worboys distinguished between regular repeat prescriptions, acute prescriptions, and repeat dispensing prescriptions:
- Regular repeat prescriptions
- These can be requested by the GP to the pharmacy for a period of 3 months. Every repeat prescription has to be generated after this period – which is something the pharmacy can do directly with the doctor. These are for patients who are stable on certain medications, not likely to be needing any changes.
- Acute prescriptions
- a one-off issue (eg painkillers after a hip operation), or when medication needs to be titrated (doses may need to be altered over time)
- Where other checks (eg blood pressure) need to be done before repeating a prescription (eg warfarin)
- for ‘controlled’ medications such as certain pain killers, or for steroids, etc. Some medications always remain on the acute list, others only temporarily.
- Repeat dispensing
- Some medications may be ordered by the doctor for a year, and dispensed by the pharmacy in three-month batches. After one year, a new dispensing prescription has to be generated.
The presentation and discussion showed how complex the system is, and how important communication between the pharmacies and the Practice is. One of the ways of addressing problems with prescriptions is through the appointment of clinical pharmacists. There should be four at the Practice, but currently there are only 1.5. A new senior clinical pharmacist is currently being recruited.
The Process Of Speaking To A Doctor
A number of patients have expressed great frustration in getting to speak to their own doctor. While they can phone and ask Reception staff to leave a message for their doctor to call them back, this will only happen if the doctor is in the Practice that day – otherwise they will be asked to call back when the doctor is next in. If the doctor is in, the call back to the patient may occur at any point of the day, leaving patients in limbo. Sometimes another doctor calls back.
It is also possible for fill in the e-consult form on-line, and a doctor will call back, but again, it will not necessarily be the patient’s named doctor.
Dr Worboys acknowledged the difficulties for patients, and said this is one of the big challenges facing the Practice, where, because of the Coronavirus pandemic, everything is having to be re-designed. The Practice is trying to provide a call back service on the same day, and to align patients with their named GPs, but this is not always possible for a host of reasons (eg self-isolating or quarantined staff; long patient lists for some doctors). She also reiterated that, although triage on the telephone is the first step, where face-to-face appointments are necessary, these are happening, and patients are going to the Practice for a number of different consultations.
3. CPPEG FEEDBACK
Issues dealt with:
- Flu vaccine is being rolled out in Camden now, through GP practices, pharmacies or three dedicated mass vaccination sites.
- Organized by HealthWatch Camden, a Questions and Answer on-line meeting took place in August, with staff from the Royal Free and University College hospitals and members of the public. Hospital staff emphasised that they had invested in providing covid-free environments, and that patients should not be afraid to go to hospital when necessary. Another meeting is planned for November 4th, between 5.30-6.30, on primary health services in Camden. More information will be sent out nearer the time.
4. GARDEN
Ian Critchley continues to keep the garden going, and more volunteers are starting. The garden is a peaceful and attractive place for patients to wait in, or to look at from the waiting room.
5. FEEDBACK FROM THE PRACTICE
Staffing changes:
- Operations Manager Sarah McDonagh has left, and the position has been taken on by Jamil Ahmed.
- New GP trainees started in August.
- Praise Kuzamba, a senior Physician Associate, has joined the Practice. Physician Associates do much of the same work as GPs, except do not prescribe. A second physician associate will start in November
Flu vaccine:
Flu clinics are all booked clinics with the 1st week being over 65yrs only, starting on 3rd October.
- Every weekday morning (except Wednesday) 08.30-10.30am;
- Every weekday afternoon 2-4pm (2.30-4.30pm on Tuesdays);
- Every Saturday 9am-3pm
- The dedicated phone number to make an appointment for the flu clinic is: 020 7428 452
6. AOB
Having these PPG zoom meetings more frequently was suggested, and considered. However, because of other commitments, it was not possible to bring forward the next meeting date which is Thursday November 26th. If issues arise in the meantime, patients should not hesitate to contact the website.

